A recent study completed by researchers with the University of Iowa Public Policy Center may help prevent future dental-care shortages in Iowa.
The policy briefs—which analyze state workforce information collected by the Iowa Dentist Tracking System (IDTS) over a 17-year period—indicate a large number of Iowa dentists are nearing retirement age, fewer dentists are practicing in rural areas, and the proportion of dentists who work in solo practice is declining.
The research is the first longitudinal look at Iowa’s dental workforce and aims to inform dental educators, workforce-development agencies, and health departments across the state about trends with the goal of collaborating to prevent gaps in access.
Did you know?
Approximately 75 percent of Iowa's dentists are graduates of the UI College of Dentistry.
That proportion has remained unchanged since 1997.
“Having a sense of what is going on statewide allows us to be more proactive in our recruitment and retention efforts,” says UI alumna Julie Reynolds, visiting assistant dental professor at the UI and co-author of the study. “No one wants to have to drive two hours to see the dentist, so collecting this data can help the College of Dentistry continue to partner with communities, proactively plan, and encourage talented students to practice in Iowa after graduation.”
The four-part study shows the proportion of Iowa dentists aged 55 and older nearly doubled—from 23 percent to 42 percent—between 1997 and 2013, meaning almost half of Iowa’s dentists are near retirement age.
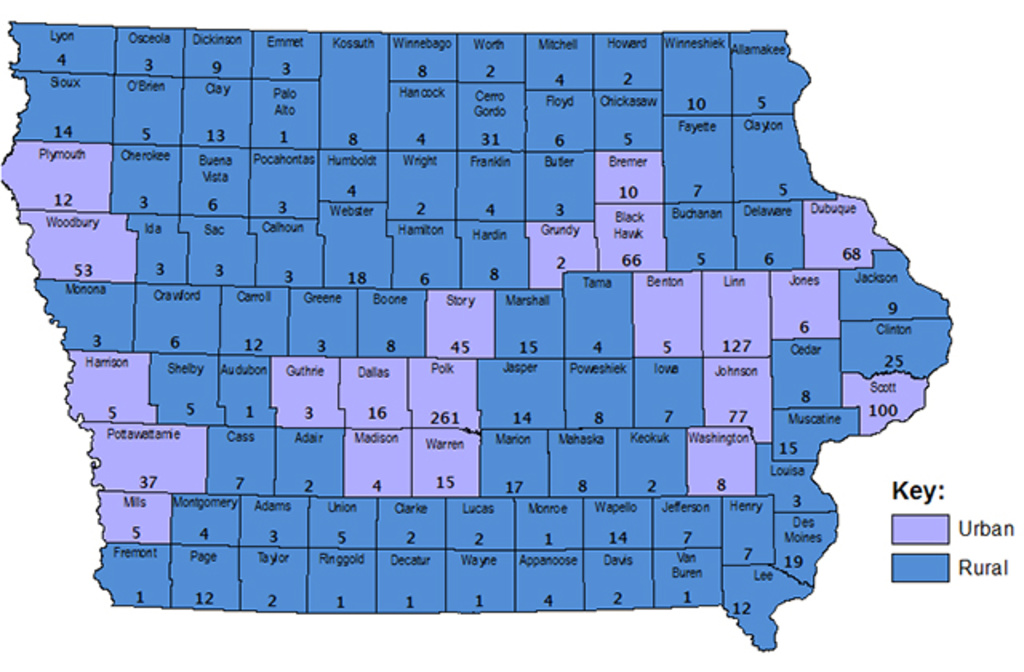
It also demonstrates that the proportion of dentists working in rural communities has decreased steadily—from 49 percent to 36 percent—and one third of Iowa’s private-practice dentists are concentrated in three metro counties. The combined population of those counties—Polk, Linn, and Scott—accounts for only 27 percent of Iowa’s population.
“These changing demographics are likely to impact overall practice patterns, as well as the geographic distribution of Iowa’s dentists,” says Raymond Kuthy, UI professor of preventive and community dentistry, adding that, as younger dentists enter the workforce, there may be a shift toward more group-based or corporate practice settings.
In fact, part of the study shows the predominate practice arrangement in Iowa shifted from solo to group practice, with the proportion of Iowa dentists who work in solo practice declining from 59 percent in 1997 to 43 percent in 2013.
“People who go into group practice tend to wind up in larger communities because it provides them with a larger patient pool, better emergency coverage in the dentist’s absence, and the ability to vary their work hours,” Kuthy says.
Kuthy speculates that this trend toward group practice—which is compounded by an increased number of dentists reaching retirement age—could threaten access to dental care in rural communities.
But that’s why this research is being done: to prepare for the future.
“We know there are health disparities, so we are trying to determine where the dentists are in terms of availability and, on the access side, what the impediments are,” Kuthy says. “By documenting which people are receiving care and which people aren’t receiving care, we can improve statewide efforts to recruit and retain dental providers to underserved communities in Iowa.”
The Office of Iowa Practice Opportunities promotes dental practice opportunities in Iowa and serves as a free resource to any Iowa community, student, or practitioner.
Its website features an interactive map for dentists seeking job opportunities in Iowa's 99 counties.
The good news is the UI College of Dentistry and Dental Clinics is already a leader in matching dental students with job openings in the state through its Office of Iowa Practice Opportunities (OIPO). Established in 2007, the office has facilitated communication between students, dentists, and communities for nearly 10 years, and is often the first place students turn when they’re deciding what to do after graduation.
As of June 30, 2015, the OIPO has helped facilitate 188 placements, 88 of which were in rural communities.
To read the study, visit the Public Policy Center website.
Primary investigators on the study were Kuthy, Reynolds, and Assistant Professor Susan McKernan. The policy brief series was funded, in part, by the Health Resources and Services Administration, DHHS (T12HP14992).